You are provided a chest x-ray and a heart recording of a 69-year-old woman (see below) but were not told anything about her history or physical examination.
What is your diagnosis, what test(s) would you order to confirm your suspicions, and what treatment, if any, do you recommend?
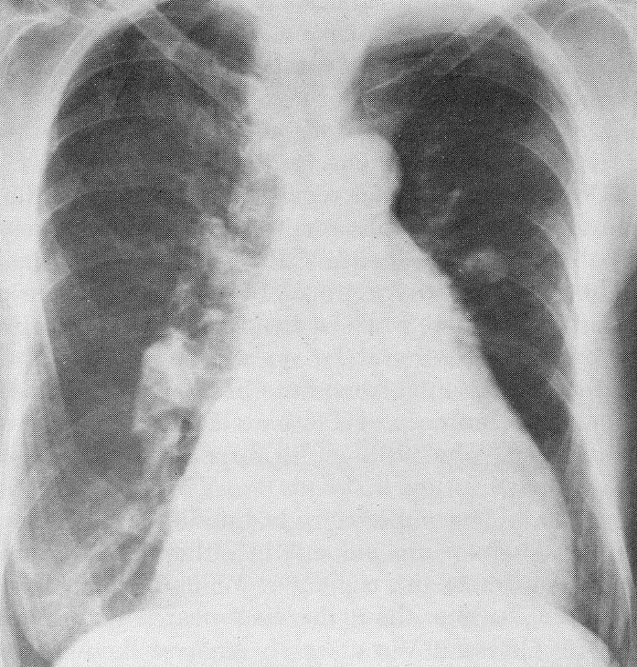
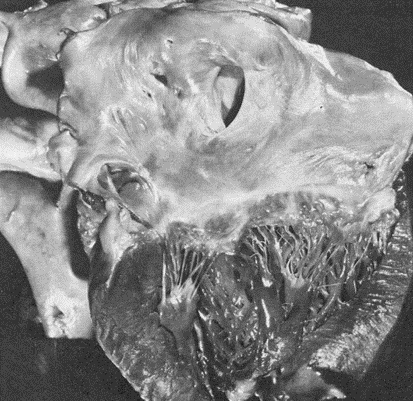
DIAGNOSIS: Atrial septal defect (ASD) (note right panel above which shows a secundum ASD) leading to severe pulmonary hypertension and reversal of the shunt (Eisenmenger syndrome).
On auscultation of the heart, this patient has the characteristic wide fixed split of the second heart sound heard best over the left second intercostal space (S2P) (click or touch left panel above to hear the murmur). The split is due to a prolonged right ventricular ejection time and increased pulmonary artery capacitance, which, in turn, delay closure of the pulmonary valve.
Left untreated, this patient developed severe pulmonary hypertension and reversal of the intracardiac shunt from left to right to right to left (Eisenmenger syndrome). The findings on her chest x-ray are characteristic of chronic pulmonary hypertension with marked enlargement of the main pulmonary artery segment and right ventricle (RVH) (note the rounded apical segment and the encroachment of the ventricle on the retrosternal space).
On physical examination, RVH is suspected whenever the right heart border extends beyond 4 cm from the midsternal line in the right 4th intercostal space, particularly when accompanied by retrosternal dullness and a left parasternal tap or thrust. As was true in the presented case, patients with Eisenmenger syndrome may show a lip color that is both cyanotic and plethoric, a result of hypoxemia and secondary polycythemia, respectively.
It is important to note that many ASDs are not discovered until adulthood. The patient may be asymptomatic or complain of exercise intolerance and dyspnea on exertion. Early intervention with closure of the defect is essential. Small secundum ASDs can often be closed with occluder devices placed percutaneously.
 Stout Drive Road Closure
Stout Drive Road Closure