A 30-year old woman presents with a chief complaint of "tender lumps" on her legs for the past week. She also notes low grade fever, malaise, and generalized arthralgias. She recently recovered from an upper respiratory tract infection. Her only medication is an oral contraceptive. Her past medical history is unremarkable.
Physical examination is notable for a temperature of 100 degrees F, a pulse rate of 85 beats/minute, a blood pressure of 125/70, and a respiratory rate of 14 breaths/minute. The exam is normal except for the presence of large, equisitely tender dusky-colored nodules on the shins of both legs (see photo below).
What is your diagnosis, what test(s) would you order to confirm your suspicions, and what treatment, if any, do you recommend?
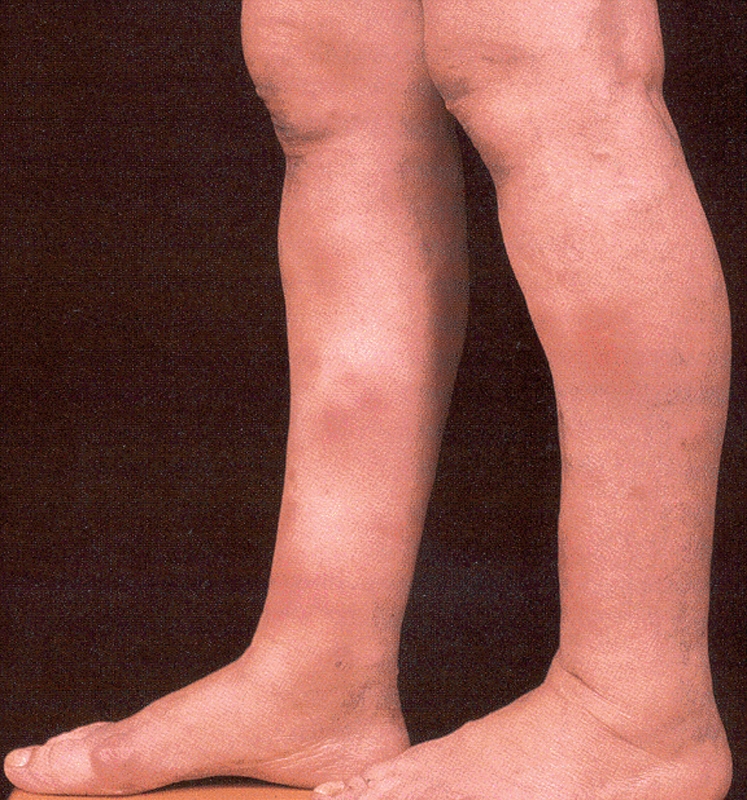
DIAGNOSIS: Erythema nodosum (EN).
Most commonly seen in females (ratio 5:1) with a peak incidence between the ages of 18 and 34 years, EN is characterized by tender large violateous nonulcerative nodules typically involving the shins, knees and ankles and, less commonly, the arms and face. The disorder is often preceded by a nonspecific prodrome of one to three weeks which may include fever, malaise, arthralgias, and symptoms of an upper respiratory tract infection.
EN may be triggered by a variety of disorders including infections due to streptococcal paryngitis (most common cause in adults), mycoplasma, tuberculosis, coccidiomycosis, leprosy, and yersinia. Granulomatous disorders (Behcet's, sarcoidosis, Crohn's disease), drugs (sulfonamides, penicillins, oral contraceptives), pregnancy, and, rarely, malignancies have also been shown to trigger EN. Between 17% and 72% of cases are idiopathic.
Histopathology shows immune complex deposition in the septal venules of subcutaneous fat causing a neutrophilic panniculitis. However, the pathological features vary with the chronology of the lesions.
Although treatment is directed toward the triggering agent, EN often resolves without treatment, the lesions fading within two to six weeks. Therefore, symptomatic support is adequate for the majority of patients. Agents used to provide symptomatic relief include nonsteroidal anti-inflammatory agents (first line) and colchicine (2nd line). Prednisone can be used for severe disease and dapsone or hydroxychloroquine for chronic or relapsing disease.
 Stout Drive Road Closure
Stout Drive Road Closure