A 35-year-old man with grade 4B Hodgkin's disease presents with a 3-day history of fever, rigors, dyspnea, a non-productive cough, and multiple skin lesions.
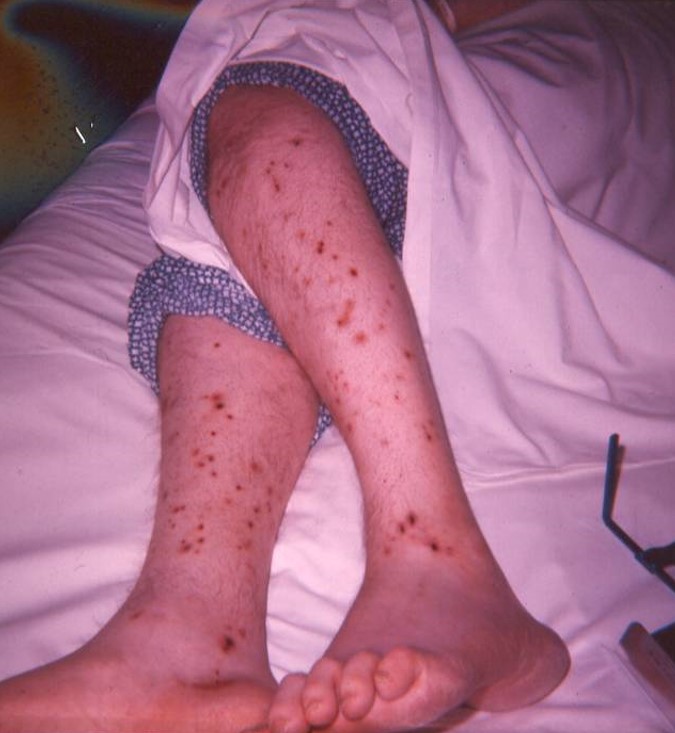
Physical examination is notable for a temperature of 38.5ºC, a pulse of 110 beats/minute, a respiratory rate of 28 breaths/minute, and a blood pressure of 110/60 mmHg. His legs are covered with multiple encrusted pustules (see panel 1 below) and his lung exam is notable for diffuse inspiratory crackles. He has a grade 3 holosystolic murmur heard loudest over the mitral area.
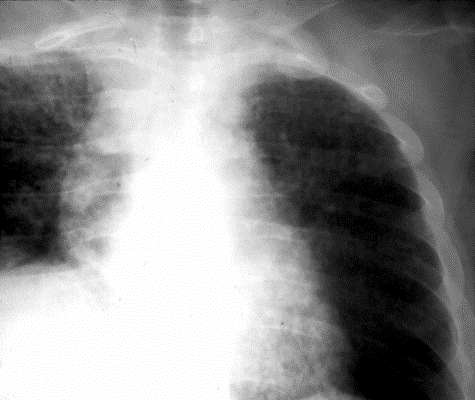
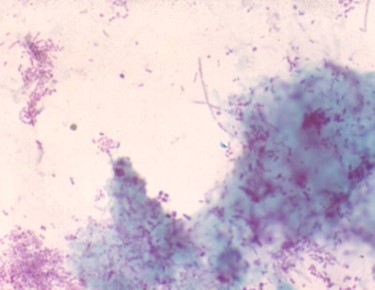
A PA of the chest shows a right hilar mass lesion and a miliary infiltrate. A modified acid fast stain of an aspirate from one of the skin lesions is shown below (see panels 2 & 3 below).
What is your diagnosis, what test(s) do you want to order to confirm your suspicions, and what treatment, if any, do you recommend?
DIAGNOSIS:Disseminated nocardiosis.
Nocardia asteroides is an opportunistic aerobic bacterium of higher order whose physical characteristics resemble those of actinomyces - a strictly anaerobic organism. Both species are Gram positive branching beaded coccobacilli, whereas nocardia is also modified acid fast positive (see right panel above). There are over a hundred nocardia species, many of which are implicated in human disease. Nocardia is a ubiquitous soil organism involved in the decay of organic materials.Nocardia usually gains entry through the lungs where it is characterized by its ability to cause a subacute pneumonia and to mimic miliary and cavitary tuberculosis and tumor (see middle panel above). In the host, with defective cell-mediated immunity, dissemination to the brain (most common), skin (see left panel above), and internal organs, may occur. In addition to his skin and pulmonary involvement, the presented case had nocardia endocarditis and a one liter abdominal wall nocardia abscess. Trimethoprim (10-20 mg/kg)-sulfamethoxazole (50-100 mg/kg) (TMZ-SMX) given in two divided doses per day is the drug of choice in most cases of nocardia infection. Daily doses TMZ-SMX doses can be reduced to as little as 5/25 mg/kg after induction therapy. For immunocompromised hosts and for those who are immunologicaly competent with brain abscesses, treatment should continue for 12 months. Pulmonary involvement in normal hosts requires 6-12 months of treatment. Unfortunately, the presented case expired despite the introduction of parenteral treatment with TMZ-SMX.
 Stout Drive Road Closure
Stout Drive Road Closure