Healthy Moms, Healthy Babies
The early years of a child’s life shape their health, learning, and well-being for years to come. When communities support mothers and babies with high-quality care before, during, and after pregnancy, they lay the foundation for healthy growth and help prevent future health problems for both mother and baby. High quality early care also strengthens bonding and supports lifelong well-being.
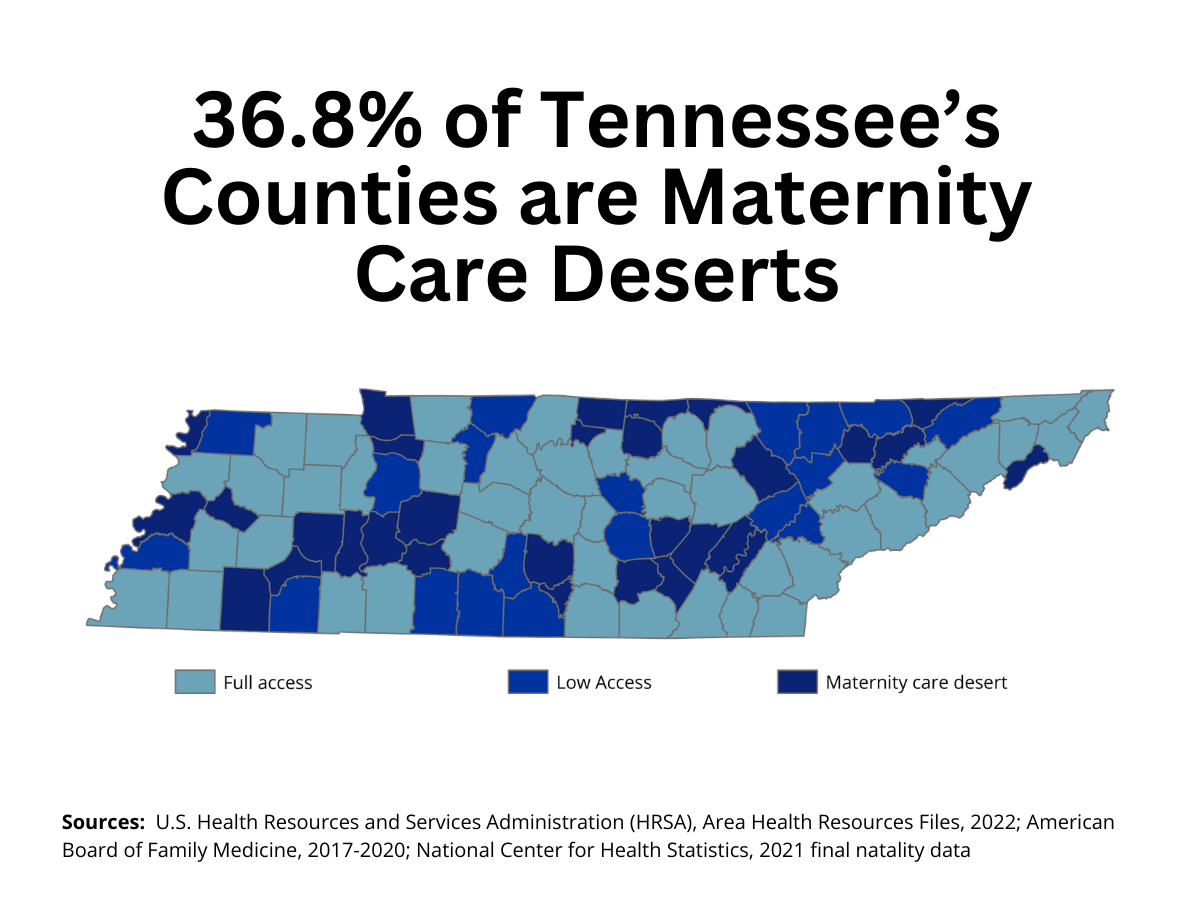
Access to care plays a significant role in the health of mothers and babies. More than one-third of Tennessee’s counties are considered maternity care deserts.1 Nearly three out of ten women must drive at least 30 minutes to receive maternity care, in part because 46 of Tennessee’s 95 counties have no practicing obstetrician-gynecologists (OB/GYNs).1,2
The point in pregnancy when women begin receiving prenatal care plays a vital role in their health and their baby’s health. The American College of Obstetricians and Gynecologists recommends starting prenatal care early in pregnancy – ideally within the first ten weeks.3
Getting early care helps health providers check for any risks and support a healthy pregnancy from the start.3 In 2024, almost 70% of Tennessee mothers who had a live birth started prenatal care in the second or third month of pregnancy, while about 3% went through pregnancy without any prenatal care.4
According to the Centers for Disease Control and Prevention (CDC), Tennessee’s maternal mortality rate of 41.1 deaths per 100,000 live births is the highest in the United States.5 Tennessee’s infant mortality rate is also higher than the United States average, 6.48 per 100,000 live births compared to 5.6 nationally.6
To give every baby a healthy start, communities can work together to support pregnant women and new moms by:
- Building a strong, shared commitment to prevention and early support
- Making prenatal and postnatal health and mental health care easier to reach
- Advocating for policies that help families thrive
When communities come together to support mothers and babies, they help create a healthier, more resilient future for all.
-
Why are Healthy Moms and Healthy Babies Important for Community Well-Being?
Supporting pregnant women and mothers of young children is an investment in our state’s future vitality. The early years of life strongly shape a child’s long-term health and development. Adverse experiences during pregnancy or childhood can have lasting effects on learning, behavior, and emotional well-being.7 On the other hand, positive experiences can help buffer stress, support healthy brain development, and lead to better relationships and stronger health throughout adulthood.8
Complications related to pregnancy can begin before, during, or after birth and may affect the mother, the baby, or both.9 Common issues such as high blood pressure, gestational diabetes, and anemia are often preventable or manageable with regular care.10 Maternal health problems can create risks for babies, including low birth weight or premature birth, which may affect early development in areas like communication, problem-solving, and social skills.11 Even with these risks, many women with health conditions have healthy pregnancies and healthy babies. Investing in maternal health throughout pregnancy is key to supporting positive outcomes for both mothers and infants during the earliest, most important stages of life.
Maternal mental health is just as important as physical health for both mothers and babies. Women often experience significant changes in their relationships and support networks during pregnancy and after birth, which can increase feelings of loneliness, isolation, and depression.12 Depression affects women at higher rates than men, and low-income pregnant and parenting women face even greater challenges in getting the care they need.13
The perinatal period encompasses the duration of pregnancy and the first year after birth—a stage marked by significant physical and emotional changes and requiring essential support.12 In Tennessee, between 2016 and 2020, 13.4% of women reported depression during pregnancy, and 17.1% reported postpartum depressive symptoms.14 Isolation and loneliness are key contributors to depression during the perinatal period, and research shows that programs helping women strengthen their support networks can reduce these symptoms.12
Untreated maternal depression can also affect a mother’s ability to care for her child. It is linked to lower rates of breastfeeding, reduced bonding between mother and infant, and a higher risk of developmental delays.15 Children of mothers with depression are more likely to experience behavioral and social challenges during their school years.16 Early screening tools help health care providers identify postpartum depression early and connect mothers to timely care that can prevent or reduce those risks.15
When communities prioritize maternal mental health, they support healthier mothers, healthier babies, and stronger, more resilient families overall.
-
What are the Disparities?
Some communities face challenges that make it harder to access needed maternal care. Barriers such as long travel distances, limited providers, high costs, and other systemic issues can complicate access to both physical and mental health services. Families in these communities often need extra support to stay healthy and ensure their children's well-being.
Rural Communities
In many rural areas of Tennessee, access to prenatal care is limited. Fewer health care facilities and long travel distances make it harder for pregnant women to get timely, consistent care. More than one-third of Tennessee counties are considered maternity care deserts, meaning they lack a hospital or birth center that provides obstetric care.1 Maternity care deserts place rural women at greater risk during pregnancy and childbirth. More than half of rural women (55.1%) live over 30 minutes from a birthing hospital.17 About 72% of Tennessee’s rural counties lack access to obstetric care, and only 44% of rural hospitals offered labor and delivery services in 2025.18,19
When women travel farther for care, the risk of maternal complications and poor infant outcomes increases. Long travel times are linked to higher rates of maternal morbidity and infant outcomes such as stillbirth and NICU admission.20 Rural women and infants experience greater health disparities when compared to those living in more metropolitan areas. According to the Pregnancy Mortality Surveillance System from the Centers for Disease Control and Prevention, risks of pregnancy-related death are highest for rural populations. In 2023, 26.8 maternal deaths per 100,000 occurred in less populated areas compared to 20.2 maternal deaths per 100,000 in larger cities or towns.21
A national study found that women living in rural areas were less likely to have a medical visit in the year before pregnancy or during the postpartum period.22 They were also less likely to receive important screening and counseling services during prenatal and postnatal care.22 In addition, rural communities have higher rates of teen pregnancy.23
Ensuring that mothers receive consistent, high-quality care during pregnancy and childbirth builds the foundation for healthier children, stronger families, and thriving communities across Tennessee.
Women Experiencing Homelessness
A national study using Pregnancy Risk Assessment Monitoring System (PRAMS) data from 2016 to 2021 found that 2.4% of postpartum women had experienced homelessness in the year before delivery.24 Even short periods of homelessness can create serious risks for pregnant women. Without stable housing, women are more likely to miss medical appointments, struggle to meet basic needs, and face higher levels of stress—all of which can affect pregnancy. As a result, pregnant women experiencing homelessness face significant health challenges that impact both their well-being and the health of their babies.
Women experiencing homelessness have higher rates of pregnancy-related complications and chronic health issues.25 Research shows they have a 1.21 times higher risk of hypertension during pregnancy, a 1.36 times higher risk of gestational diabetes, and a 1.83 times higher risk of postpartum depression.24 They are also more likely to experience multiple pregnancy complications and have high rates of mental illness and substance use disorders.26

Unhoused pregnant women are less likely to receive timely prenatal care, to breastfeed, or to attend well-baby checkups.27 Babies born to women experiencing homelessness are more likely to have a low birth weight, be born early, or need neonatal intensive care, which often leads to longer hospital stays.28 Infants born to mothers who experienced homelessness during pregnancy are also at higher risk for neonatal abstinence syndrome, hypoxic-ischemic encephalopathy, and necrotizing enterocolitis.29 These health challenges can continue into childhood and adulthood, increasing the risk for long-term health issues and higher health care costs.25
Uninsured Women
When women lack health insurance, they often struggle to access prenatal and postnatal care, which can lead to poorer health outcomes for both mothers and babies.30,31 Without regular checkups, essential health issues can go untreated, increasing risks during pregnancy and after childbirth. A recent systematic review found that women with comprehensive health insurance were more likely to attend postpartum visits and had fewer preventable hospital readmissions and emergency department visits.32

However, access to health insurance remains a challenge for many mothers. A national study of Medicaid-covered new mothers using data from 2015 to 2018 found that 26.8% were uninsured before pregnancy and 21.9% were uninsured 2 to 6 months after birth.33 Another national study of community health centers found that 6.4% of pregnant women were uninsured for their entire pregnancy.30 A similar study using data from 2015 to 2018 reported that about 11.5% of new mothers were uninsured.33 Women who lose pregnancy-related Medicaid coverage in the postpartum period face a higher number of unmet health care needs.34
In Tennessee, these challenges are significant. In 2022, about one in eight women (12.9%) were uninsured before pregnancy, and 7.3% were uninsured after pregnancy.35 Uninsured women, especially those without consistent perinatal care, face increased risks during pregnancy and after childbirth. Women without insurance are 4.75 times more likely to die from pregnancy-related complications than women with private insurance.36
Lack of insurance also affects infants. Newborns without insurance have a higher risk of low birth weight and infant mortality.37 Even among mothers with insurance, outcomes vary depending on the type of coverage. A national study from 2017 to 2020 found that infants born to mothers with Medicaid had higher infant mortality rates than those born to mothers with private insurance, 5.30 versus 2.75 deaths per 1,000 live births.38 These infants also had higher rates of low birth weight, preterm birth, and the mothers were less likely to receive first-trimester prenatal care.38
Racial and Ethnic Minorities
Not all mothers in Tennessee have the same access to safe, high-quality care. Gaps in health care access, income, and treatment contribute to racial and ethnic differences in maternal and infant health. National studies show rising rates of hypertensive disorders of pregnancy, chronic hypertension, and diabetes among Hispanic and non-Hispanic Black women.39
In Tennessee, differences in prenatal care are clear. From 2022 to 2024, more than one in three Hispanic mothers (34.5%) did not receive pregnancy-related care until the fifth month of pregnancy or later.40 The rates were about one in four for American Indian/Alaska Native (AI/AN) mothers (24.2%) and Black mothers (24.2%), about one in six for Asian/Pacific Islander mothers (16.7%), and about one in eight for White mothers (12.4%).40
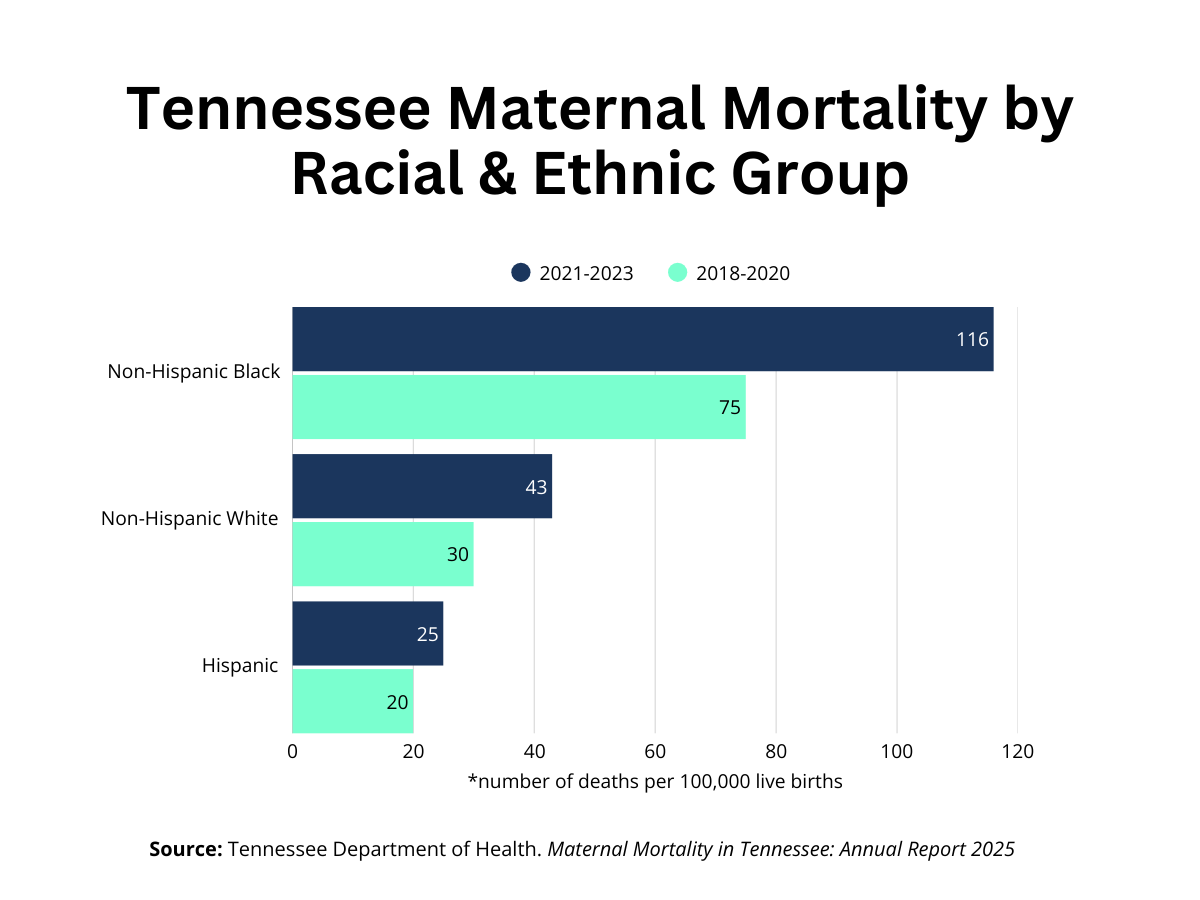
Pregnancy-related deaths continue to show serious racial differences in Tennessee. Between 2021 and 2023, Non-Hispanic Black women experienced the highest pregnancy-related mortality rate at 116 deaths per 100,000 live births, nearly three times higher than the rate among Non-Hispanic White women.41 Between 2019 and 2021, Tennessee experienced a 124% increase in pregnancy-related deaths, driven in part by the COVID-19 pandemic and updated practices by the state’s Maternal Mortality Review Committee (MMRC).41 Rates then improved, decreasing by 15% in 2022 and another 25% in 2023.41 Although pregnancy-related deaths declined after the COVID-19 pandemic, these differences remain. Among Black women, cardiovascular conditions were the leading cause of pregnancy-related death (31%).41 Mental health conditions were the leading cause of pregnancy-related death across all racial and ethnic groups (27%).41
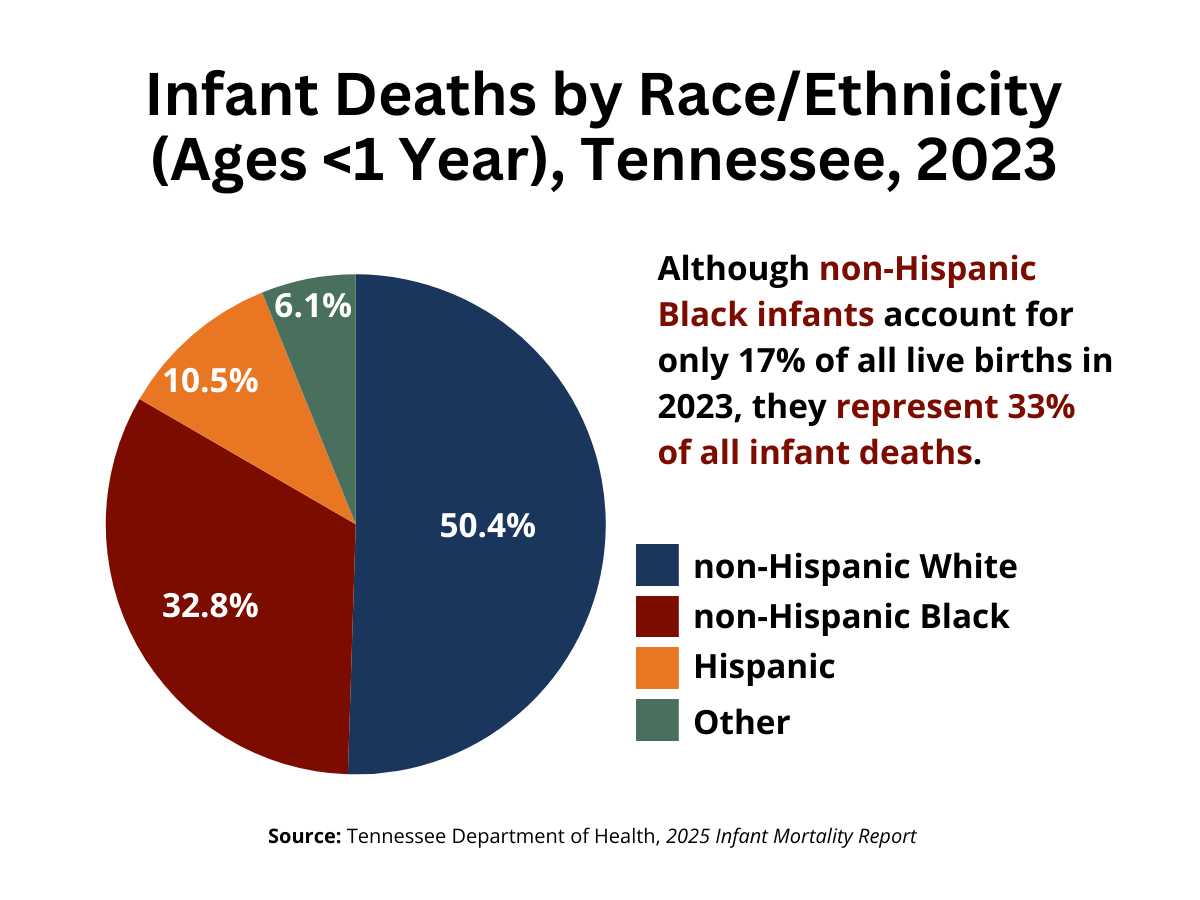
These differences do not end with mothers—they also affect babies. In 2023, about one in 81 Black infants in Tennessee died before their first birthday (12.4 per 1,000 live births), compared to about 1 in 192 White infants (5.2 per 1,000).42 Although non-Hispanic Black infants accounted for only 17% of all live births in 2023, they represented 33% of all infant deaths.42 Black infants continue to face more than twice the risk of infant death compared to White infants.42 These differences reflect ongoing gaps in access to care, maternal health conditions, and broader social and economic factors that affect families across Tennessee.
Teen Parents
Teen pregnancy can create serious challenges for young mothers and their babies. It is associated with higher health risks for both mother and baby, lower high school graduation rates, and long-term economic instability.43 Teen mothers are more likely to experience pregnancy and delivery complications, including preterm birth, low birth weight, and infant death.44 They also experience higher rates of depression before and after birth.45 Postpartum depression affects about one in 16 teen mothers (6.1%), compared to about one in 26 adult mothers (3.8%).46
Teen pregnancy affects more than health. It also shapes the broader social and behavioral challenges young parents face. Teenage pregnancy is also associated with higher rates of substance use.47 These risks can also affect a teenage parent’s ability to finish high school.44

In 2023, Tennessee had the sixth-highest teen birth rate in the country, with about two births for every 100 teen girls (20.4 births per 1,000 females ages 15-19).48 Hispanic teens had the highest birth rate in Tennessee, at about 4 per 100 teens (42.9 per 1,000 females ages 15–19).49 Black teens had the second-highest rate at about three in 100 teens (29.9 per 1,000 females ages 15-19).49

Teen pregnancy is often connected to broader life circumstances. Adolescents who grow up in poverty — especially those who experienced maltreatment — are at higher risk of becoming teen parents.50 Childhood poverty is also linked to teenage pregnancy, and teen pregnancy can also make it harder to escape poverty.51 Teen pregnancy is also more common among teens in foster care. About one in two young women in foster care has given birth by age 20.52 Many youths in foster care experience instability, trauma, and limited access to consistent health care and supportive adult relationships, which can increase their risk of teen pregnancy.
Children born to teen mothers are more likely to face health concerns, learning challenges, and social-emotional difficulties.44 They are also more likely to become teen parents themselves.44 These patterns show why prevention and early support are so important.
-
Community-Driven Solutions
Community-driven solutions are practical steps that local partners can take together to support mothers and babies. These actions are evidence-informed, achievable in the short term, and designed to address the most critical needs in each community.
- Raise Awareness and Educate
- Launch public education campaigns to promote the importance of prenatal and postpartum care.
- Spread awareness of local and state maternal health programs and support services.
- Educate families about urgent maternal warning signs during pregnancy and after birth.
- Provide information about healthy nutrition, exercise, prenatal vitamins, and managing chronic health conditions during pregnancy.
- Increase education about perinatal mental health for both patients and health care providers.
- Improve Access to Support Programs
- Connect families to government resources such as TennCare (Medicaid), CoverKids (CHIP), WIC, and Community Health Access and Navigation in Tennessee (CHANT).
- Host workshops to help families navigate enrollment in assistance programs.
- Collaborate with local WIC offices to increase access to breastfeeding support, nutritious foods, infant formula, and health care referrals.
- Help eligible pregnant women enroll in Presumptive Eligibility (PE), which provides immediate, temporary TennCare coverage for prenatal, delivery, and postpartum care. PE is available at county health departments across the state and can help women start care right away.
- Support Teen Parents and Prevent Teen Pregnancy
- Provide education for teens and young adults on comprehensive sexual risk avoidance and family planning.
- Increase community awareness of adolescent pregnancy prevention strategies.
- Promote Breastfeeding and Early Support
- Expand community-based breastfeeding support programs to increase breastfeeding rates. Breastfeeding helps protect infants from illness and supports maternal health during and after pregnancy.
- Partner with Evidence-Based Home Visiting (EBHV) programs to provide in-home parenting support, education, and referrals.
- Host community baby showers to connect expecting parents with supplies, local resources, and family-based services.
- Expand Perinatal Support Services
- Integrate doula services into community care systems. Pregnant and postpartum women who receive doula care have improved health outcomes for themselves and their infants, including higher breastfeeding initiation rates, fewer low-birthweight babies, and lower cesarean delivery rates.
- Increase transportation support for families impacted by maternity care deserts.
- Promote group prenatal care, where a small group of expecting mothers can gather to receive education, support, and peer connection facilitated by a health professional.
- Incorporate maternal care initiatives into homelessness services to ensure pregnant women experiencing homelessness receive essential care.
- Build partnerships to increase access to perinatal care, including mental health and substance use disorder treatment, especially for incarcerated women and other vulnerable populations.
- Strengthen Perinatal Mental Health Support
- Encourage open conversations about mental health during pregnancy and after birth.
- Create safe community spaces and referral pathways for women experiencing perinatal depression or anxiety.
- Stay Connected
- Sign up for the Tennessee Maternal Health Matters Newsletter to stay informed about maternal health trends, best practices, and learning opportunities. The newsletter is the monthly go-to source for maternal health professionals, delivering the latest trends, events, best practices, and learning opportunities each month to your inbox. To sign up for the newsletter, click here.
- Raise Awareness and Educate
-
Making Change Through Policies and Systems
Policy and systems change focuses on how health care providers, public health agencies, and community partners work together to improve maternal and infant health. When systems are better connected, families can access care more easily and receive consistent support. This section outlines evidence-informed, long-term strategies to strengthen care systems and achieve lasting improvements for moms and babies.
- Engage in Statewide Leadership
- Join the Maternal Health Task Force (MHTF), a multidisciplinary group overseen by the Tennessee Department of Health and open to Tennessee residents committed to improving maternal health. Members represent health care providers, mental health professionals, doulas, community organizations, TennCare, and patient advocates. The task force advances strategies aligned with Maternal Mortality Review Committee recommendations and fosters statewide collaboration to strengthen care before, during, and after pregnancy. Click here to learn more or join the MHTF.
- Strengthen Economic Supports for Families
- Connect eligible community members to financial assistance programs such as SNAP, WIC, and childcare subsidies.
- Champion federal and state economic policies that improve financial security and stability for families. Provide resources to communities that highlight the importance of these economic policies to support babies and parents.
- Encourage employers to offer paid parental leave and sick leave so parents can recover and bond without financial strain.
- Improve Mental Health and Social Support
- Advocate for universal screening for mental health conditions and social needs during and after pregnancy.
- Share evidence-based guidance, such as recommendations from the American College of Obstetricians and Gynecologists.
- Create safe spaces where mothers feel comfortable talking about mental health challenges.
- Support Family Planning and Education
- Encourage schools to provide family planning education that helps young people make informed decisions.
- Promote awareness of the Tennessee Department of Health family planning programs.
- Share information about services available through all 95 county health departments, including birth control counseling, cancer screenings, emergency contraception, and pre-pregnancy counseling.
- Expand Access to Quality Childcare
- Support high-quality early childhood care by encouraging the licensing and accreditation of childcare programs.
- Advocate for funding that helps childcare centers strengthen services and improve outcomes for young children.
- Stay informed about statewide progress
- Build on recent momentum. The 2025 Maternal Mortality Annual Report found that nearly three out of four pregnancy-related deaths in 2023 may have been preventable.41 Tennessee has launched a Maternal Health Strategic Plan focused on improving mental health care, strengthening emergency and cardiovascular care, addressing substance use, and reducing social barriers to care. Communities can support this progress by staying informed, sharing resources, and working together to ensure every mother receives respectful, high-quality care.
- Engage in Statewide Leadership
-
Community Spotlight
The Health Council Community of Practice (CoP) connects Tennessee Health Councils through shared learning and discussion around health priorities. The links below provide access to recent CoP conversations related to this topic. To learn more about the Community of Practice, click here.
Submit your own Community Spotlight! Please email Health.Councils@tn.gov with any relevant stories, resources, or presentations related to this topic.
-
Partners and Resources
Tennessee Department of Health
- Adolescent Pregnancy Clearinghouse
This website provides information on statewide programs and services, online training opportunities, and state and national data on adolescent pregnancy. For additional assistance, contact the Teen Pregnancy Information Clearinghouse toll-free line at 877-461-8277. - Adolescent Pregnancy Prevention Program
This state-funded program promotes awareness and prevention of teen pregnancy through education, community partnerships, and coordinated services. It works to reduce teen pregnancy rates and strengthen support for pregnant teens and teen parents. - Breastfeeding in Tennessee
This resource shares information about the health benefits of breastfeeding for both mothers and babies and connects families to breastfeeding education and local support services across the state. Families can learn about available programs, community resources, and ways to get help throughout their breastfeeding journey. - Tennessee Breastfeeding Hotline (855-4BF-MOMS | 855-423-6667)
The Tennessee Breastfeeding Hotline is available 24 hours a day, 7 days a week in both English and Spanish. Staffed by International Board-Certified Lactation Consultants (IBCLCs), the hotline provides free support for breastfeeding concerns such as milk supply, pain, pumping, and weaning, and connects families to local lactation and WIC support services. - Doula Services Advisory Committee
This committee advises the Tennessee Department of Health on professional standards and reimbursement recommendations for TennCare-covered doula services. - Evidence-Based Home Visiting (EBHV)
EBHV programs provide in-home parenting education and support to strengthen families and improve maternal and child health. Research shows these programs improve child development, family stability, and school readiness. - Fetal and Infant Mortality Review (FIMR)
FIMR is a community-based program that reviews fetal and infant deaths to identify gaps in care and improve services for mothers and babies. The program brings local partners together to develop strategies that strengthen systems and reduce preventable infant deaths. - Growing Inside Free of Tobacco and Smoking (GIFTS)
GIFTS is Tennessee’s Pregnancy Tobacco Cessation Program. It provides resources and support to help pregnant women quit smoking. Quitting reduces the risk of premature birth, low birth weight, and secondhand smoke exposure for babies and children. - Maternal Health Innovation Program
This federally funded program supports state-specific strategies to reduce disparities and improve maternal health outcomes in Tennessee. - Maternal Violent Death Prevention Program
This program works to reduce maternal suicide and homicide through education, screening, partnerships, and improved data collection. - Newborn Screening Program
The Tennessee Newborn Screening Program tests all newborns for certain serious health conditions shortly after birth. Early detection through screening helps ensure that babies with these conditions receive timely follow-up care, treatment, and services that support healthy growth and development. - Perinatal Regionalization Program
This program coordinates care for pregnant women and newborns with life-threatening conditions by connecting them to specialized Regional Perinatal Centers across Tennessee. - Tennessee Infant Safe Sleep Program
This program promotes safe sleep practices by distributing educational materials and portable cribs, and by encouraging parents to place infants alone on their backs in a crib. - Tennessee Maternal Mortality Review and Prevention Program
This program reviews maternal deaths and develops strategies to prevent future deaths and improve maternal health outcomes statewide. The program includes the Maternal Mortality Review Committee (MMRC), a multidisciplinary panel that reviews deaths during pregnancy and within one year after pregnancy and makes recommendations to improve policies and care. It also includes the Maternal Health Task Force, an open, statewide group of health care providers, community organizations, mental health professionals, doulas, TennCare representatives, and patient advocates who collaborate to implement prevention strategies and strengthen care before, during, and after pregnancy. - Women, Infants, and Children (WIC)
WIC provides healthy foods, nutrition education, breastfeeding support, and referrals to health and community services for eligible pregnant, postpartum, and breastfeeding women, infants, and children up to age five.
Tennessee Commission on Children and Youth
- The Tennessee Commission on Children and Youth is an independent, nonpartisan agency that works to ensure state policies and programs promote and protect the health, well-being, and development of children and youth.
Tennessee Department of Intellectual & Developmental Disabilities
- Family Support Program
The Family Support Program helps families of children and adults with disabilities access information, services, and individualized supports that promote independence and community participation. The program offers service coordination, support planning, and referrals to resources that help families meet long-term needs. - Tennessee Early Intervention System (TEIS)
TEIS is a voluntary program that provides therapy and support services for infants and young children with developmental delays or disabilities. Services are provided at no cost to families.
Tennessee Department of Mental Health and Substance Abuse Services
- Housing and Homeless Services
This program provides resources to help individuals and families find housing and access support for mental health and substance use needs. - Services for Children and Youth
This statewide program provides crisis support and intervention for children and adolescents experiencing behavioral health emergencies. Services include 24/7 crisis assessment, stabilization, and links to community resources to help children and families stay safe and get timely help during emotional or mental health crises. - Tennessee Redline (800-889-9789)
The Tennessee Redline is a 24/7 referral service that connects individuals and families to addiction treatment and recovery services. - 988 Suicide & Crisis Lifeline
This free, confidential 24/7 support line is for anyone experiencing mental health or emotional distress, including thoughts of suicide, self-harm, or other crises. People can call or text 988, or chat at 988lifeline.org, for themselves or for a loved one who may need crisis support. Trained counselors provide immediate support, crisis de-escalation, and connections to local mental health services.
Tennessee Division of TennCare
- TennCare Kids
TennCare Kids provides comprehensive checkups and health care services for children from birth through age 20 who are enrolled in TennCare. - Presumptive Eligibility (PE)
The Presumptive Eligibility program provides immediate, temporary TennCare coverage for eligible pregnant individuals so they can begin prenatal and other health care services right away. Coverage extends through at least one year postpartum. - CoverKids (CHIP)
CoverKids is Tennessee’s Children’s Health Insurance Program (CHIP), which provides low-cost or free health coverage for eligible uninsured children and pregnant women.
- FindHelpNowTN.org is an online directory that connects individuals to substance use treatment and recovery services across Tennessee. Users can search for available services in near real time based on treatment type, payment options, and location.
- Kid Central TN is a one-stop resource for Tennessee families raising children from birth to age 18. The website provides information on child development, health, education, and access to state-supported services.
Mothers’ Milk Bank of Tennessee
- The Mothers’ Milk Bank of Tennessee is a nonprofit organization that provides safe, pasteurized donor human milk to medically vulnerable infants who need it most.
- Nurses for Newborns is a free home visitation program that partners with families to ensure babies are safe and healthy while building caregiver confidence and support.
Tennessee Initiative for Quality Perinatal Care (TIQPC)
- TIQPC works to improve the quality of care for mothers and babies across Tennessee. Through collaborative learning and quality improvement efforts, the program helps reduce pregnancy complications and strengthen perinatal care practices.
- Healthy Mom Healthy Baby Tennessee Podcast (TIQPC)
This podcast, produced by the Tennessee Initiative for Quality Perinatal Care (TIQPC), features conversations with providers and experts across the state working to improve maternal and infant health. Episodes highlight topics such as racial disparities, perinatal care improvements, and the opioid crisis affecting Tennessee families.
To Learn More:
Centers for Disease Control and Prevention
- HEAR HER Campaign
The CDC’s HEAR HER Campaign raises awareness about urgent maternal warning signs during pregnancy and the year after birth. The campaign encourages families and health care providers to listen to mothers’ concerns and act quickly to prevent pregnancy-related deaths. - Perinatal Quality Collaboratives (PQCs)
PQCs are state- and multi-state partnerships that bring together health care teams to improve care and outcomes for mothers and babies. They use data and quality improvement strategies to reduce complications, improve birth outcomes, and address disparities in maternal and infant health.
Centers for Medicare & Medicaid Services
- Integrated Care for Kids (InCK) Model
This innovation strengthens care coordination for children enrolled in Medicaid and CHIP by integrating physical and behavioral health, as well as community services. By improving early identification of health needs and connecting families to the right supports, InCK helps promote healthier outcomes for children from infancy through early childhood. - Maternal Opioid Misuse (MOM) Model
The MOM Model is an initiative that improves care coordination for pregnant and postpartum Medicaid enrollees with opioid use disorder. The model supports state-led efforts to reduce care fragmentation and improve outcomes for mothers and babies.
- Cherished Mom works to support pregnant and postpartum women, their families, and perinatal health care providers by raising awareness about Perinatal Mood and Anxiety Disorders (PMADs), including postpartum psychosis and maternal suicide prevention. The organization provides education, resources, and community support to reduce stigma and help families access mental health care.
Health Resources & Services Administration (HRSA) Maternal and Child Health
- Alliance for Innovation on Maternal Health (AIM)
AIM is a national quality improvement initiative that brings together hospitals, clinicians, public health leaders, and community partners to implement evidence-based safety bundles that improve care and reduce preventable maternal complications and deaths across the United States. - Healthy Start
Healthy Start is a federally funded program that supports pregnant women, new mothers, and families in communities with high infant mortality rates. It provides outreach, care coordination, health education, and connections to prenatal and postpartum services to help improve birth outcomes, reduce infant deaths, and strengthen family support systems.
- March of Dimes is a nonprofit organization dedicated to improving the health of mothers and babies. The Tennessee chapter offers education, advocacy, and resources to prevent premature birth and support healthy pregnancies.
- Mother of Fact is a digital health platform that connects mothers and families with registered dietitians to provide personalized nutrition support for pregnancy and early childhood.
National Maternal Mental Health Hotline (833-TLC-MAMA | 1-833-852-6262)
- This free, confidential 24/7 hotline offers support before, during, and after pregnancy. Callers can receive real-time counseling, referrals to local and telehealth providers, and connections to support groups. Services are available in English and Spanish, with interpreter services in more than 60 languages.
- NICU Helping Hands provides education and support to families with infants in the Neonatal Intensive Care Unit (NICU), during the transition home, and in the event of infant loss.
Postpartum Support International (PSI)
- Postpartum Support International provides education, peer support, and connections to trained professionals for individuals experiencing perinatal mental health challenges. PSI offers resources for families and health care providers to improve early identification and treatment.
- Adolescent Pregnancy Clearinghouse
 University Commons
University Commons 